
Opioid Prevention Education
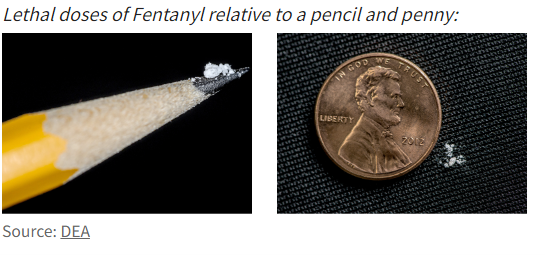
Opioid deaths in California have increased over the last three years, with 6,095 opioid fatalities related to fentanyl in 2022. Fentanyl is a powerful synthetic opioid that is challenging to detect and increases the likelihood of an overdose. California has recently seen xylazine, a tranquilizer that has not been approved for human use, present in some opioid overdoses.
Awareness of the risks associated with opioid use and overdoses, as well as community resources and primary prevention education, are vital to substance use prevention work. Important efforts to prevent opioid overdose include medication safe storage and disposal practices and opioid use and misuse prevention education training. When harm reduction funding sources are available, some primary preventionists, in collaboration with intervention and treatment partners, might also have access to options such as test strips and overdose education training.
Safe Storage/Disposal Practices:
Engaging in medication safe storage and disposal practices can help prevent the use and misuse of prescription medication. Safe storage practices include checking for and disposing of expired medication, keeping medication out of access from children and those at risk of use or misuse, and further securing narcotics and other substances in locked cabinets or drawers.
California’s Drug Take-Back Program provides resources and education on proper medication disposal, and many pharmacies participate in drug take-back services, such as these pharmacies in California.
Test Strips:
Test strips are available across California for both fentanyl and xylazine. Understanding the myths vs. facts about fentanyl can help people make important decisions about testing drugs before use. While not a primary prevention strategy under the Substance Abuse and Mental Health Services Administration’s (SAMHSA) primary prevention strategies, access to test strips can be an important partner strategy for primary preventionists working with professionals who implement intervention and treatment strategies under the Institute of Medicine’s (IOM) Continuum of Care.
Overdose Training:
A similar intervention and harm reduction strategy, Naloxone, can be used to reverse an opioid overdose. To increase access to Naloxone and reduce overdoses and fatalities, California has a statewide standing order for providers to access Naloxone. Individuals can use the National Harm Reduction Coalition’s Naloxone Finder to locate suppliers. SAMHSA has a comprehensive Opioid Overdose Prevention Toolkit with information for first responders, prescribers, patients, and family members. This is a great resource for primary preventionists who are interested in participating with professionals who are funded to implement harm reduction strategies.

American Indian Heritage Month
November marks the start of American Indian Heritage Month. This time of recognition began as American Indian Day by Seneca Indian Dr. Arthur C. Parker in Rochester, N.Y. In 1990, President George H. W. Bush designated November as “National American Indian Heritage Month,” which has continued annually under varying names since 1994.
1.7% of California’s population is American Indian or Alaska Native. California is home to approximately 110 recognized tribes and is the state with the 3rd highest American Indian population. American Indians face unique risk factors that influence substance use disorders and behavioral health concerns, but rich traditions and connections within families and tribal communities prove to be effective protective factors.
The Gathering of Native Americans/Alaska Natives (GONA/GOAN) is a planning framework created by SAMHSA’s Tribal Training and Technical Assistance Center. The process focuses on highlighting Belonging, Mastery, Interdependence, and Generosity and the Indigenous Theoretical Framework of Vision, Circles of Relationships, and Sense of Hope. The GONA/GOAN helps members understand the impact relationships can have on resilience and how they can leverage community resources to impact prevention.
Traditions, wisdom, and cultural practices are passed down through generations. The Haudenosaunee (Iroquois) Seven Generations Principle aims to preserve land and cultural practices so that the following seven generations can thrive. This is used to guide ecological practices as well as strengthen individual relationships and wellbeing.
For additional resources about prevention in Native American populations in California, see below:
- The Sacramento Native American Health Center
- Sierra Native Alliance
- United American Indian Involvement, Inc.

Veteran’s Day
November 11th marks Veteran’s Day, when the nation honors those who served in the United States Armed Forces. California has one of the highest military populations in the United States – it is home to nearly 30 military bases and 1.8 million veterans. CalVet, the California Department of Veteran’s Affairs, offers a variety of services to veterans and their families including mental health resources, but fewer than 50% of veterans use any Veterans Affairs (VA) Services at all.
According to the CDC, suicide is the leading cause of death among veterans under the age of 45, and the 13th leading cause of death for veterans overall. The CDC is using research on suicide data to inform the Comprehensive Suicide Prevention Program, which aims to use a public health approach to foster resilient and healthy communities. In 2018, the U.S. Department of VA released a ten-year strategic plan for preventing veteran suicide through promoting wellness, enhancing preventative services, and research.
Substance use disorders (SUDs) are higher among veterans than the general population. SUDs are associated with increased risk factors including suicide, medical issues, co-morbid psychiatric diagnoses, and challenges with maintaining employment and housing. By increasing wellness and key protective factors, challenges with SUDs can be reduced.
It’s important to note that prevention work includes not just Service Members and Veterans, but also their Families (SMVF). 50% of Active Duty members are married, and 35.4% have children. Extended leave impacts the behavioral health of military family members, especially children. By expanding access to health services to military families, we can address the effects of stress on SMVF
Protective Factors for Suicide Prevention:
https://www.cdc.gov/suicide/factors/index.html
- Healthy coping skills
- Feeling connected with others – partners, friends, family, community
- Availability of physical and behavioral healthcare, including access to substance use treatment
- Reduced access to lethal means of suicide
